Researchers at Nagoya University report that two common gut microbes can work together to break down the colon’s protective mucus layer, leaving stool dry and difficult to pass—an effect that standard laxatives may not address. The team also found higher levels of these bacteria in people with Parkinson’s disease, who often experience constipation decades before motor symptoms, and showed in mice that disabling a key bacterial enzyme prevented constipation.
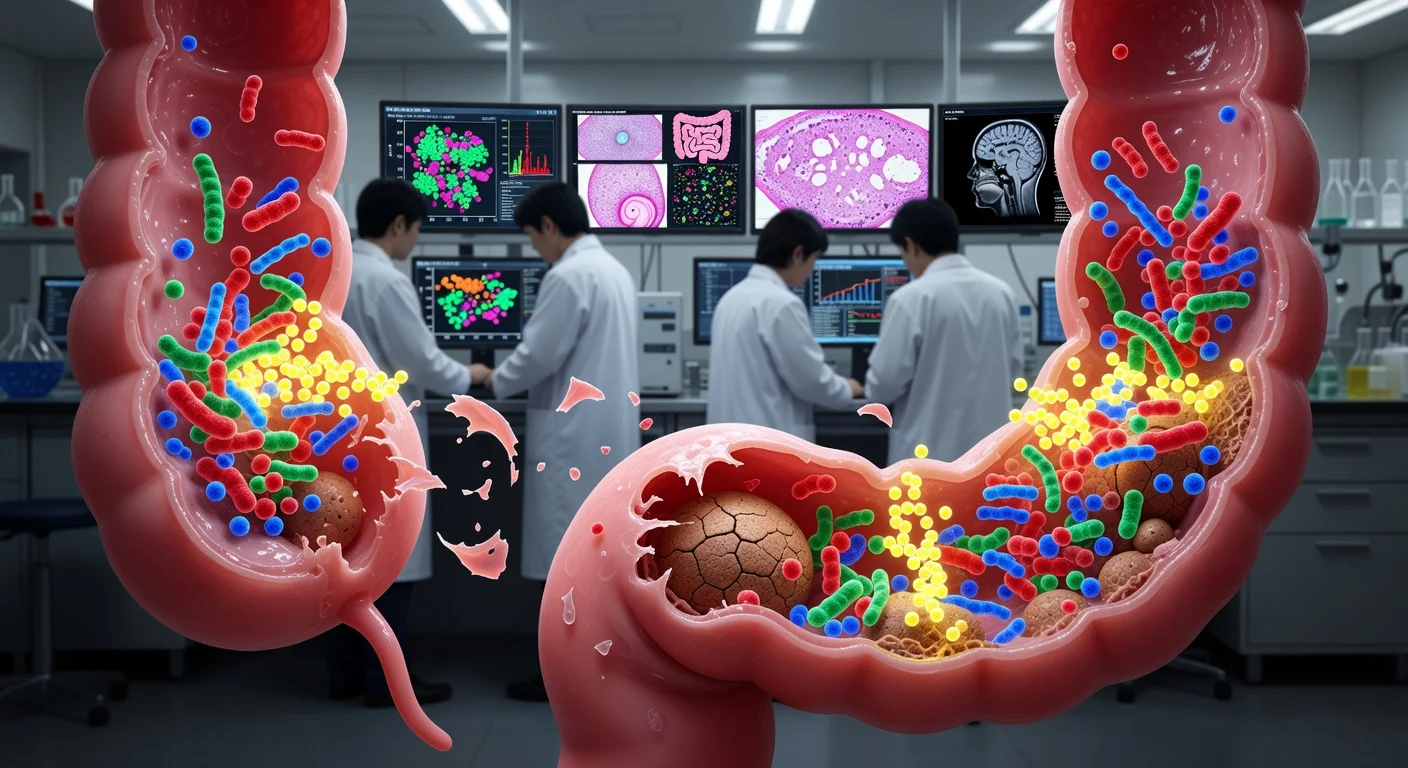
Scientists at Nagoya University in Japan have identified two gut bacteria that appear to work in tandem to promote chronic constipation by eroding the colon’s protective mucus layer. The research, published in the journal Gut Microbes, focuses on Akkermansia muciniphila and Bacteroides thetaiotaomicron, which the researchers say can break down the mucus coating that helps keep the colon lubricated and stool hydrated.
According to the researchers, the mucus loss unfolds in stages. B. thetaiotaomicron produces enzymes that remove sulfate groups from mucin—chemical features the team says normally help protect mucin from being broken down. Once those sulfate groups are removed, A. muciniphila can more readily digest the exposed mucin. As mucin levels fall, stool can lose moisture and become harder and more difficult to pass.
The work is positioned as a possible explanation for why some people with persistent constipation do not respond well to standard therapies that primarily aim to soften stool or stimulate intestinal movement. The Nagoya group highlights chronic idiopathic constipation—constipation without a clear underlying cause—as an area where focusing on the mucus barrier and microbiome could be particularly relevant.
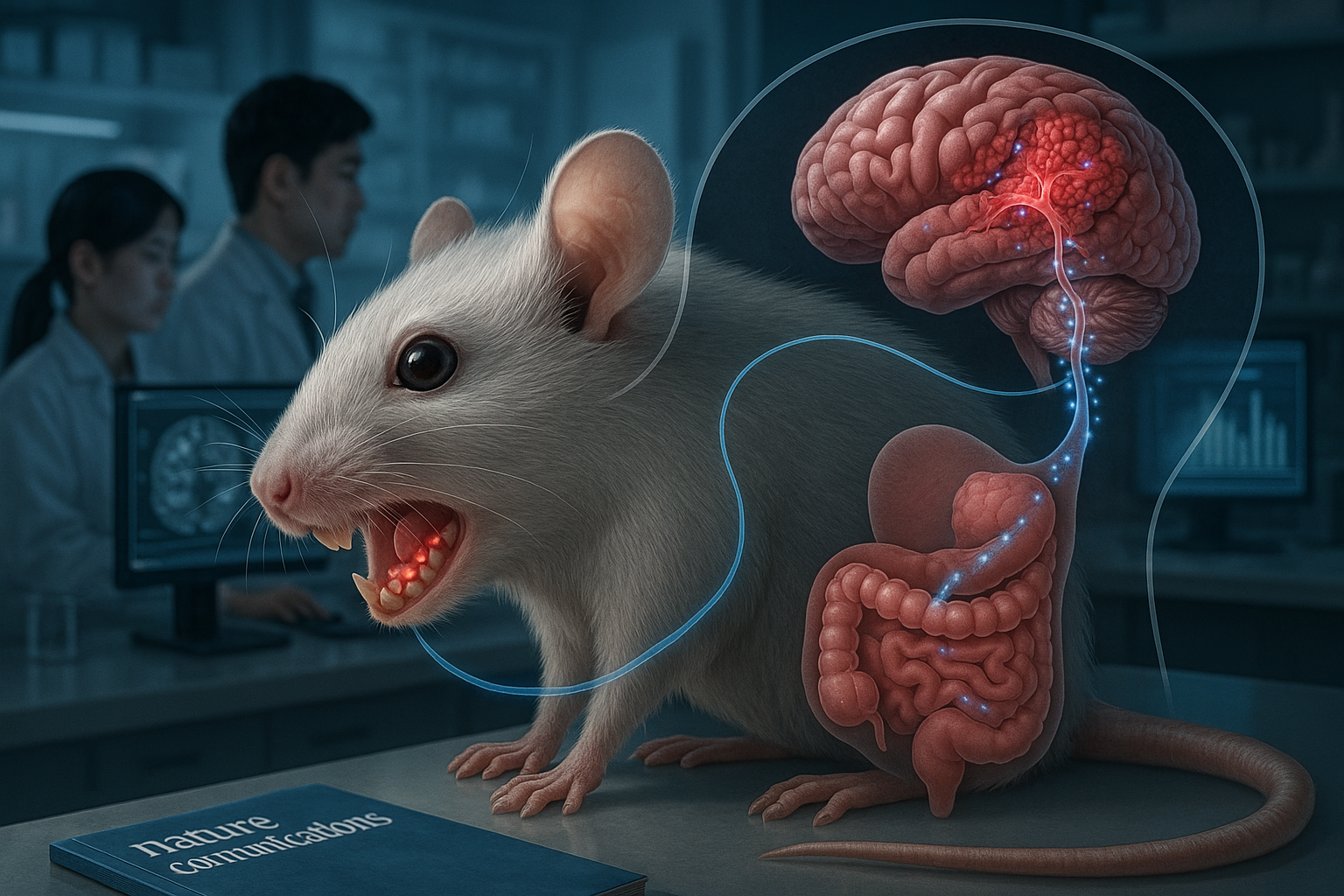
The team also reports a connection to Parkinson’s disease. Parkinson’s patients often experience constipation long before the emergence of hallmark movement symptoms, and the researchers found higher levels of these mucus-degrading bacteria in Parkinson’s patients. While constipation in Parkinson’s disease has frequently been attributed to neurological changes, the findings suggest that bacterial activity in the gut could also contribute to early gastrointestinal symptoms.
To test whether interrupting the process could prevent constipation, the researchers genetically modified B. thetaiotaomicron so it could no longer activate the enzyme sulfatase involved in removing sulfate groups from mucin. Lead author Tomonari Hamaguchi said: “We put these modified bacteria into germ-free mice together with Akkermansia muciniphila, and surprisingly the mice did not develop constipation; the mucin stayed protected and intact.”
In the mouse experiments, disabling that enzyme prevented the bacteria from degrading mucin and prevented constipation, the researchers reported. The team argues that the results point to sulfatase as a potential drug target, though they emphasize that translating the approach to humans would require further study.
More broadly, the findings add to growing research interest in how the gut microbiome may influence digestive symptoms and neurological disease—particularly as constipation can precede Parkinson’s motor symptoms by decades in some patients.