Millions worldwide suffer from osteoarthritis, yet many miss out on the most effective treatment: exercise. Experts highlight that movement nourishes joints and reduces pain more than surgery or medications in many cases. Studies show fewer than half of diagnosed patients receive referrals for physical activity programs.
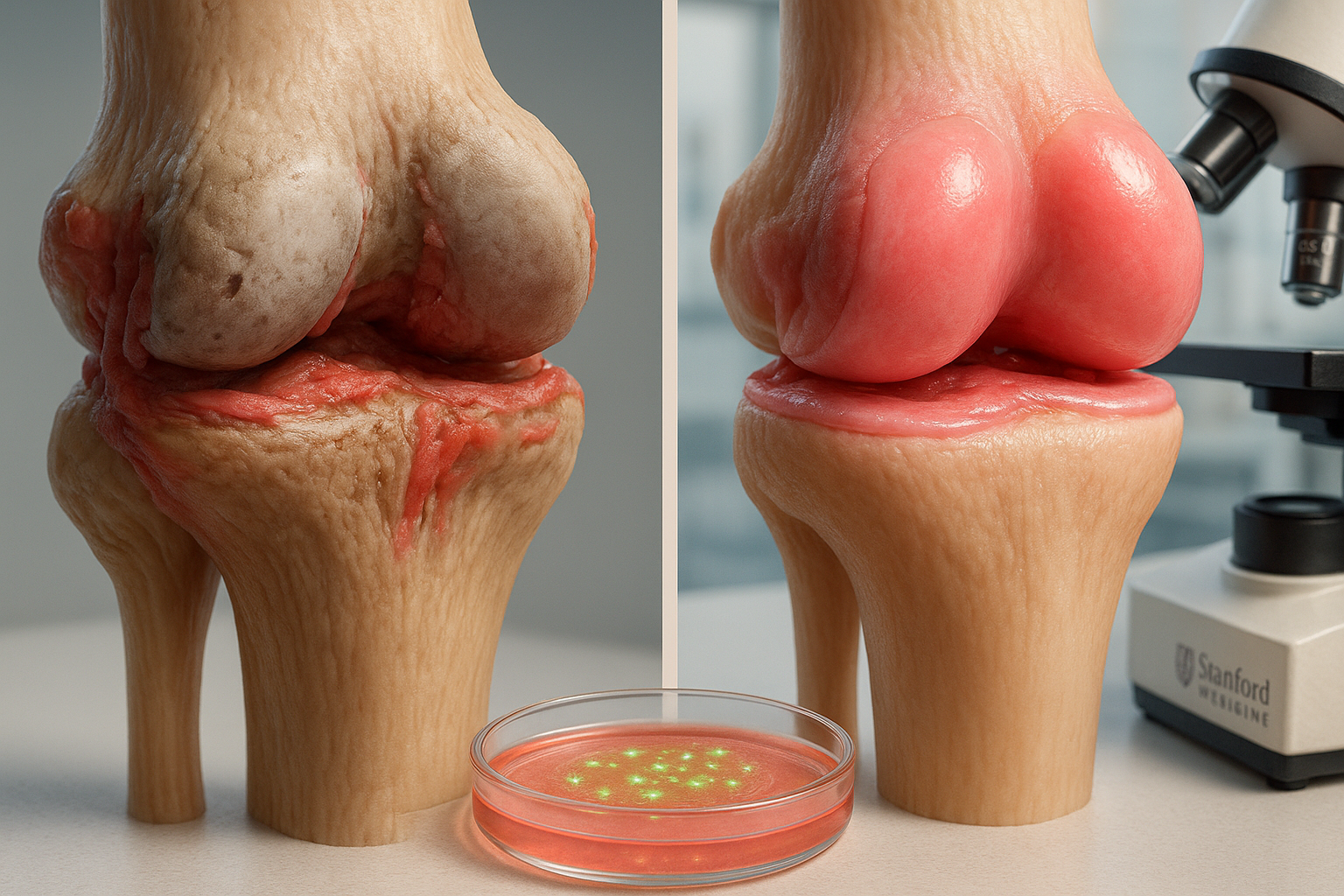
Osteoarthritis affects more than 595 million people globally and could reach one billion by 2050, driven by longer lifespans, sedentary lifestyles, and rising obesity rates. The condition involves the entire joint, including cartilage, fluid, bone, ligaments, muscles, and nerves, rather than just wear and tear.
Cartilage lacks its own blood supply and relies on movement to stay healthy. When joints are compressed during activities like walking, fluid is pushed out, and upon release, it draws in nutrients and lubricants. This process supports repair and maintenance, countering the disease's progression.
Despite evidence that exercise strengthens muscles, reduces inflammation, and improves joint function, it is underutilized. Research from Ireland, the UK, Norway, and the United States indicates that fewer than half of osteoarthritis patients are referred to exercise or physical therapy by primary care providers. Over 60 percent receive non-recommended treatments, and about 40 percent are sent to surgeons before exploring non-surgical options.
Programs like GLA:D, designed for hip and knee osteoarthritis, involve supervised group sessions focusing on movement quality, balance, and strength. Participants report reduced pain, better function, and improved quality of life for up to 12 months post-program. Exercise also addresses obesity-related inflammation by lowering markers and influencing gene expression to support joint health.
No medications alter osteoarthritis's course, and while surgery helps some, it carries risks. Experts, including Clodagh Toomey from the University of Limerick, emphasize exercise as a first-line, low-risk approach that benefits overall health across chronic conditions.