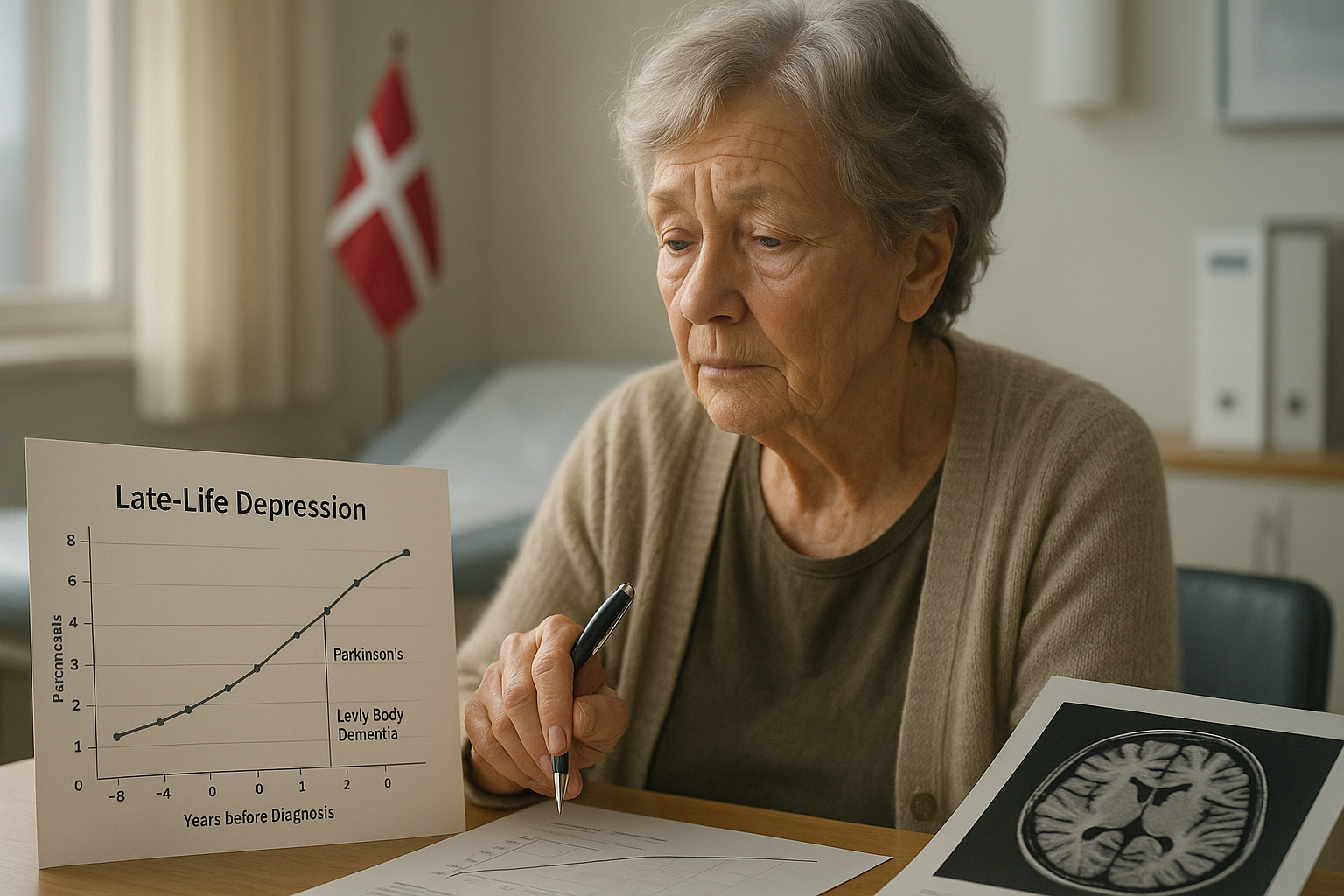
Depression diagnosed for the first time in older adults was more common in the years leading up to a diagnosis of Parkinson’s disease or Lewy body dementia and remained elevated for years afterward, according to a large Danish registry study. The authors said the pattern—stronger than in several other chronic illnesses—supports the possibility that depression can be an early feature of these neurodegenerative conditions rather than only an emotional response to disability.
Researchers in Denmark used national health registers to conduct a retrospective, matched case–control study of 17,711 people diagnosed with Parkinson’s disease (PD) or Lewy body dementia (LBD) between 2007 and 2019. Each patient group was matched by age, sex and calendar year of diagnosis to up to three people diagnosed with other chronic conditions—rheumatoid arthritis (RA), chronic kidney disease (CKD) or osteoporosis—to compare patterns of incident depression over time.
Across the years before diagnosis, people who went on to develop PD or LBD had higher rates of newly diagnosed depression than the comparison groups, with the excess risk rising gradually and most pronounced in the roughly three years immediately before diagnosis, the study reported. The study also found that the elevated incidence persisted after diagnosis, with higher depression rates continuing for several years compared with the matched chronic-disease groups.
The authors said the contrast with RA, CKD and osteoporosis—conditions that can also involve long-term disability—suggests the increase in depression around PD and LBD diagnoses is not fully explained by the psychological burden of chronic illness alone. Instead, they wrote, the findings are compatible with depression being an early manifestation of the neurodegenerative changes that later lead to PD and LBD.
The pattern appeared stronger in LBD than in PD, with higher depression rates observed in LBD both before and after diagnosis, particularly in the years closest to the diagnosis date. The researchers noted that differences in disease course and underlying neurobiology could contribute to the gap.
“Following a diagnosis of PD or LBD, the persistent higher incidence of depression highlights the need for heightened clinical awareness and systematic screening for depressive symptoms in these patients,” first author Christopher Rohde said in a statement. He added: “Thus, our main conclusion—that PD/LBD are associated with a marked excess depression risk preceding and following diagnosis when compared with other chronic conditions—remains valid.”
The authors stressed that depression does not mean someone will inevitably develop Parkinson’s disease or Lewy body dementia. They said, however, that new-onset depression later in life may warrant closer clinical attention—both to treat depression and to support earlier recognition of possible neurodegenerative disease.
The study was published in General Psychiatry (2025; 38(6): e102405) and posted online in December 2025.