Researchers at LMU Munich, Bonn-Rhein-Sieg University of Applied Sciences, TU Darmstadt and Nanion Technologies report that the lysosomal ion channel TMEM175 helps prevent excessive acidification inside lysosomes, a malfunction that the team says could contribute to toxic buildup associated with Parkinson’s disease. The findings were reported in the Proceedings of the National Academy of Sciences.
A team from Bonn-Rhein-Sieg University of Applied Sciences (H-BRS), Ludwig Maximilian University of Munich (LMU Munich), TU Darmstadt and Nanion Technologies has reported new evidence clarifying how the lysosomal ion channel TMEM175 influences acidity in lysosomes—membrane-bound compartments that break down cellular waste.
Lysosomes need an acidic interior to degrade macromolecules into reusable building blocks. According to the researchers, this acidity is generated by a protein that pumps protons (H+) into lysosomes, while additional proteins in the lysosomal membrane help keep the pH within an optimal range.
In a study described by LMU Munich in a university news release and reposted by ScienceDaily, the scientists say TMEM175 acts as an “overflow valve” that helps prevent lysosomes from becoming too acidic. The release says the work addresses a long-running debate over whether TMEM175 primarily conducts potassium ions or protons, reporting that the channel can conduct both and that its behavior changes depending on luminal acidity.
The collaboration was led by pharmacologist Professor Christian Grimm (LMU Munich) and Dr. Oliver Rauh (H-BRS), according to the same release. The researchers said they relied largely on patch-clamp measurements—an electrophysiology method used to characterize ion flow through channels—to show that TMEM175 can sense when lysosomal acidity reaches a critical state and adjust proton flow through the channel.
In the release, Rauh is quoted as saying the study establishes a “decisive” role for TMEM175 in this process and calling the protein unusual among ion channels. “We’ve now been able to demonstrate that TMEM175 not only conducts potassium ions, but also protons, and is thus directly involved in the regulation of pH … in the interior of lysosomes,” he said.
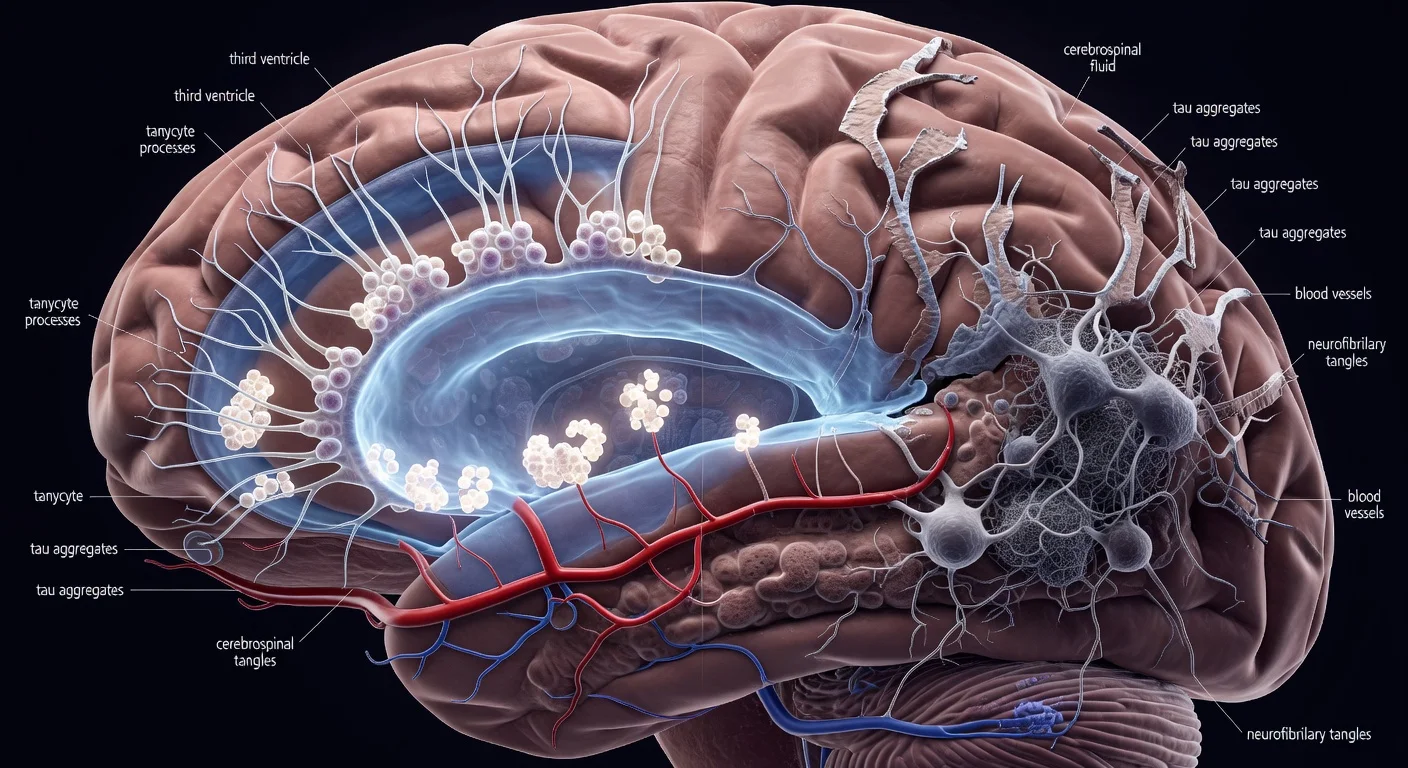
The researchers also argued that mutations affecting TMEM175 can disrupt pH regulation and impair lysosomal degradation, potentially contributing to toxic protein buildup and neuronal cell death. The news release links these effects to Parkinson’s disease and other neurodegenerative conditions and describes TMEM175 as a potential target for drug development.
The study was published in the Proceedings of the National Academy of Sciences under the title “Proton-selective conductance and gating of the lysosomal cation channel TMEM175,” with the DOI 10.1073/pnas.2503909123, and a publication date of January 14, 2026.