Northwestern University researchers say they developed an advanced lab-grown human spinal cord organoid model that reproduces key features of traumatic injury—such as inflammation and glial scarring—and that an experimental “dancing molecules” therapy reduced scar-like tissue and promoted nerve-fiber growth in the model.
Scientists at Northwestern University report they have created a highly developed human spinal cord organoid—miniature tissue grown from induced pluripotent stem cells (iPSCs)—designed to model traumatic spinal cord injury in human-like tissue. The organoids measured several millimeters across and were developed over several months to include key cell types such as neurons and astrocytes. The team also reported incorporating microglia, immune cells in the central nervous system, to better capture inflammatory responses after injury.
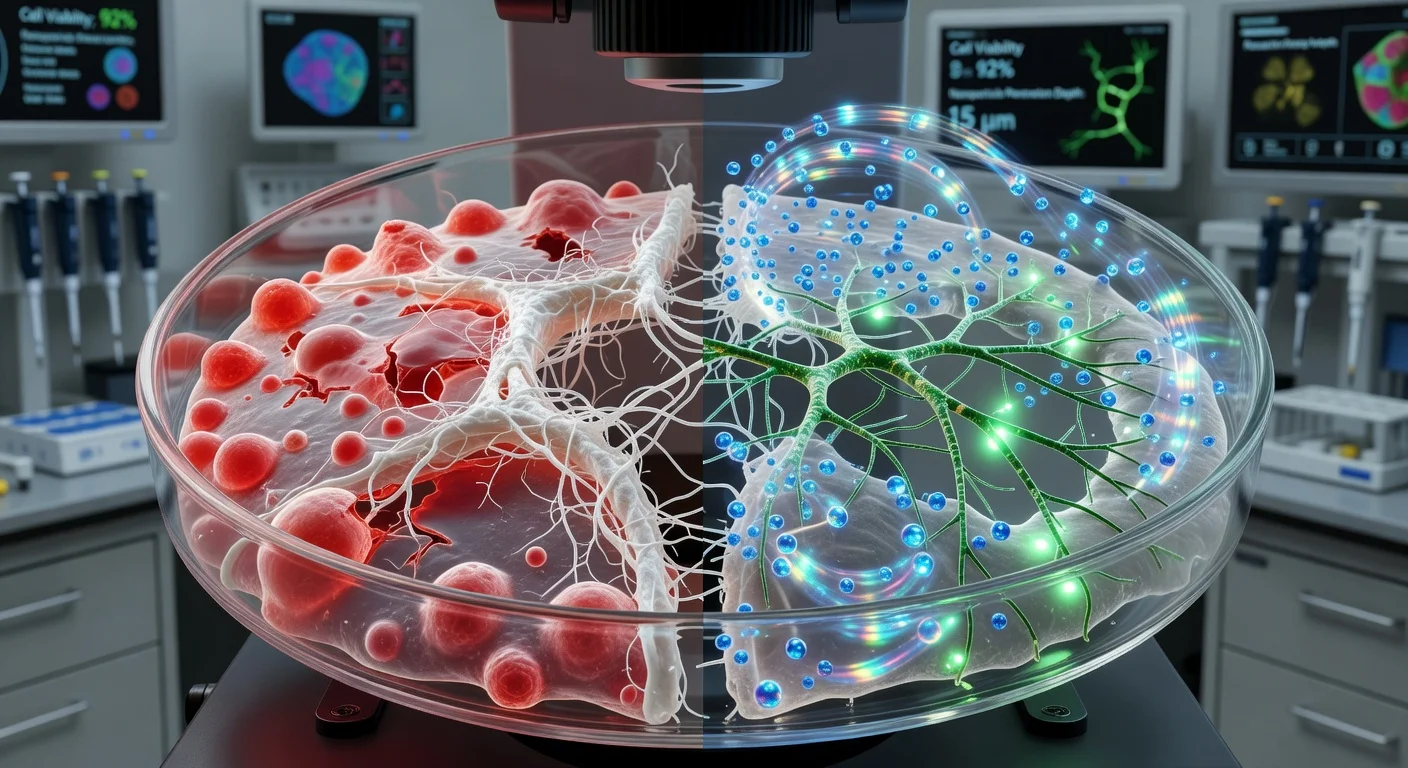
In experiments described by the university and in the peer-reviewed paper, the organoids reproduced several biological hallmarks associated with spinal cord trauma, including cell death, inflammation and glial scarring. To model different forms of injury, the researchers induced two damage patterns: a scalpel cut intended to mimic laceration-type injury and a compressive impact intended to resemble contusion injuries commonly seen in events such as serious falls or vehicle crashes.
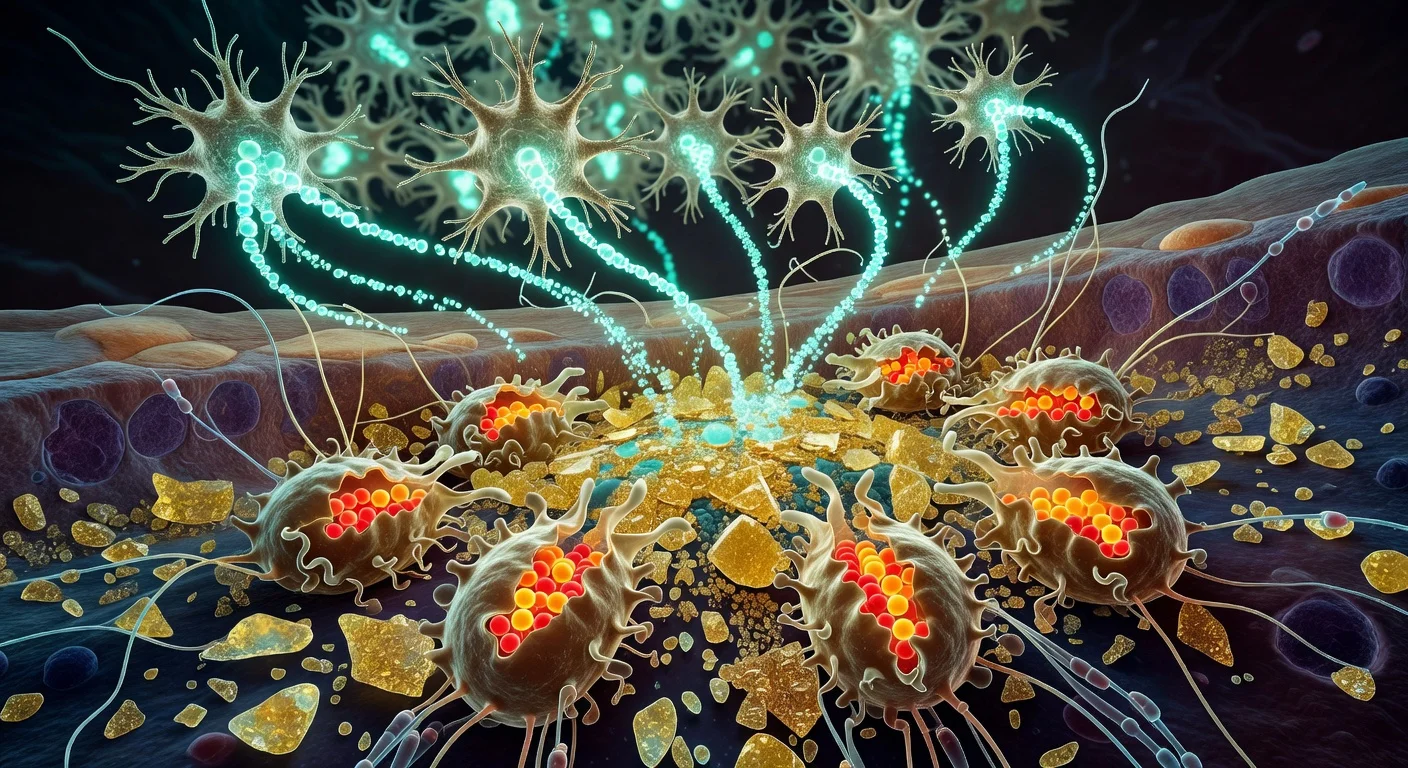
The researchers then tested an experimental injectable material they call “dancing molecules,” a supramolecular nanofiber-based therapy first reported by the same Northwestern group in 2021. The therapy is delivered as a liquid that forms a gel-like nanofiber scaffold; the group attributes its biological activity in part to rapid molecular motion that may enhance interactions with cellular receptors.
According to Northwestern, treated injured organoids showed increased neurite outgrowth—the growth of neuron extensions that include axons—and reduced scar-like tissue and inflammation compared with untreated injured organoids. “One of the most exciting aspects of organoids is that we can use them to test new therapies in human tissue,” said Samuel I. Stupp, the study’s senior author and the inventor of the “dancing molecules” platform. Stupp said that after treatment, the glial scar “faded significantly to become barely detectable,” and neurites grew in a pattern he said resembled axon regeneration previously seen in animals.
Northwestern also pointed to earlier preclinical work in mice, reported in 2021, in which a one-time injection administered 24 hours after severe spinal cord injury was associated with restored walking within four weeks. The university has said the therapy received Orphan Drug Designation from the U.S. Food and Drug Administration for acute spinal cord injury.
The organoid-injury study was published on February 11, 2026, in Nature Biomedical Engineering. Stupp is a Board of Trustees Professor at Northwestern and director of the Center for Regenerative Nanomedicine. The paper’s first author is Nozomu Takata, a research assistant professor of medicine at Northwestern’s Feinberg School of Medicine and a member of the center. While the findings suggest the approach could help evaluate regenerative strategies in human-derived tissue, the work remains preclinical and does not by itself demonstrate clinical benefit in patients.